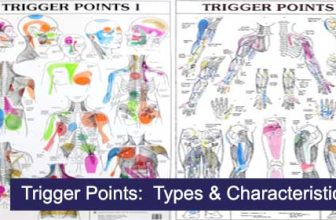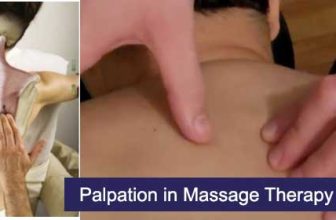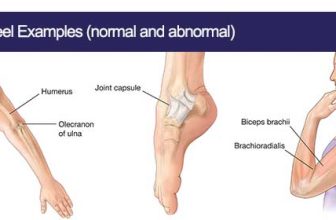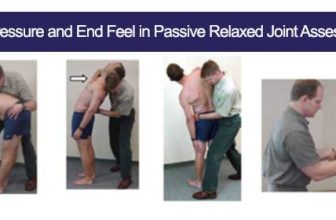
SOAP (an acronym for Subjective, Objective, Assessment, and Plan) is a method of documentation employed by health care providers including massage therapists to write out notes in a patient’s chart. A Massage Therapist’s duty is to assess and treat physical dysfunction and pain of the soft tissue and joints of the body – and SOAP notes help in accomplishing this.
* If this is the patient’s first treatment visit, the massage therapist will get the patient to fill out a confidential Medical Health History Form.
soap notes for massage therapyPurpose of SOAP Notes in Massage Therapy:
- helps organize the massage treatment plan
- to record the massage treatment purpose, plan and progress
- the SOAP note is considered a legal document, it can be used for third parties (medicare, insurance etc.)
- protects the massage therapist if the patient have any concerns regarding their care
- reinforce massage treatment progress
- used for referral and communication purposes with the patient’s other health care providers
- used for dismissal purposes (closure of the treatment)
- can be used for research and draw conclusions about massage treatments
SOAP Notes for Massage Therapy
SUBJECTIVE Component:
The subjective component of the SOAP note is initially the massage therapy client’s chief complaint. This is a statement of the client’s purpose for getting a massage therapy treatment. See (Massage Client Interview – OSCE Station 2)
The history or state of experienced symptoms are recorded in the patient’s own words. The Subjective component of the SOAP Notes include the following:
Subjective Component: Mnemonic: LORDFICARAH
- Location – location of the pain and tenderness
- Onset – when the pain started
- Referral- if the pain refers to a different area
- Duration – how long the pain lasts
- Frequency – how often the pain is felt, temporal pattern- constant, comes and goes, every morning
- Intensity – or severity of the symptom – you can use the 1-10 pain scale
- Character – the character of the pain – shooting, sharp, dull, achy etc.
- Aggravating Factors – what makes the pain worse – drugs, activity, posture etc.
- Relieving Factors – what makes the pain decrease – drugs, activity, posture etc.
- Alternative Healthcare – other medical professionals that the patient goes to, especially for this symptom – MD, chiro, physio, OT etc.
- History – health history form
*** more Health History Client Interview Mnemonics
- How has the client responded since their last massage therapy treatment?
- Specific outcome markers (ADL- activities of daily living, Pain scale)
SOAP Notes for Massage Therapy
OBJECTIVE Component:
The objective component of the soap notes in massage therapy include:
- Massage Therapist’s clinical observation – The patient’s posture (how the patient is sitting, standing), walking (gait), patient’s pain expression (pain scale).
- MD diagnosis, x-rays
- 4T’s of palpation
- Temperature – using the back of the massage therapist’s hand – tissue heat may indicate inflammation, cool indicates ischemia
- Texture – does the muscle have an even texture throughout? are sections adhered or fibrosed? presence of scar tissue, unusual moles? are there trophic changes in the skin, swelling, edema, crepitus?
- Tenderness – point tenderness on a particular structures, are the structures too painful to palpate? is pain and tenderness refer elsewhere?
- Tone – is the muscle hypertonic or flaccid? consistent throughout the muscle group?
ASSESSMENT Component:
Assessment Component of Massage Therapy SOAP Notes:
To target the cause of the patient’s symptom and to create the best possible treatment plan, the massage therapist needs to do an assessment and record the results. The assessment component includes the massage therapy client’s following:
- Gait Assessment
- Postural Assessment
- Range of Motion – see ROM Testing
- Special Tests / Orthopedic Tests – see Orthopedic Testing
Basically, the results from objective assessment
PLAN Component:
Massage Therapy SOAP Notes: (P) Plan Component
- After (1)listening to the massage therapy patient’s symptoms in the patient’s own words ( subjective component) and (2) reading/ understanding the patient’s health history form by communicating with the patient, (3) Observing the patient (4) Assessing the patient through ROM and Orthopedic testing, the massage therapist will be ready to make a well-informed Massage Treatment Plan. The Treatment Plan includes the plans for the (a) initial treatment and (b) follow-up assessment (result of the massage treatments), (c) client feedback and (d) succeeding treatments – time, date, duration.