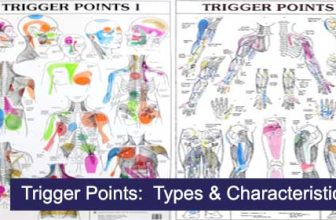
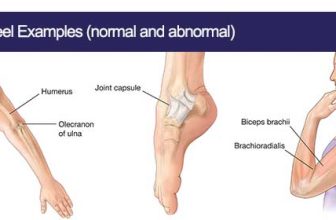
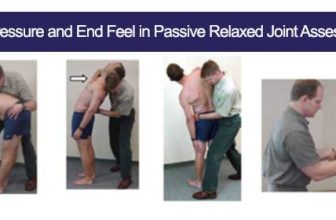
Client Health History Interview Mnemonics
A massage client’s health history interview is an important tool in helping a massage therapist devise a proper treatment plan. The following interview mnemonics help cover all the important questions needed in gathering information about the massage client’s condition.
LOC-Q-SMAT
Location
- Where? Point to it
- Write as accurate a location as possible (“low back” is too general, “lumbosacral” is better, “shoulder” is too general, “anterior & lateral right shoulder is better”)
- Always indicate right or left
- Does it radiate? Where? How far? (elbow, wrist, hand, fingertips?)
- What aspect/surface? (lateral/medial/posterior)
Onset (what happened & when?)
- When did it happen? Gradual or sudden? What caused it?
- What is the mechanism of injury? – Look for specific actions, changes in activities, posture, (worker’s compensation)
Chronology/Timing (symptom patterns)
- Constant or intermittent (episodic)
- If constant, is it truly 24 hours a day? Does it prevent sleep?
- If intermittent: is it associated with specific circumstances? (e.g., eating certain foods? Certain activities? Time of day?)
- Frequency & duration of the episodes
- Diurnal patterns (worse in morning? end of day?)
- Is there night pain (wake or prevent sleep?)
- Getting worse (progressive)? Getting better? Staying the same?
- Prior history: has this ever happened before? When? How long? What did you do about it?
Quality
- Ask patient to describe symptoms in their own words, use patient’s words in quotations
- Describe pain or symptoms (sharp, dull, etc.)
Severity/effect on ADL (activity daily living)
- Pain mild, moderate or severe?
- Pain scale (0-10)
ADL (activity daily living): can you go to work? Affect performance? Affect hobbies? Sexual activity? Simple activities such as putting on a shirt? Get specific activities & how patient is affected (excellent source of functional outcome markers)
Modifying factors
- What increases the symptoms or pain? Be specific
- What makes it better? Avoiding what? Changing posture? Rest? Medications, supplements, botanicals (dose & frequency?)
Associated symptoms
- Do you have any other symptoms or problems that you feel are related to this complaint?
- Additional specific questions are asked based on what the patient presents with & what the examiner thinks it could be; for example:
- Neck or back complaint, is there numbness, tingling, or weakness in an extremity?
- Low back: does your back ever catch or get locked? Change in bowel habits? Change in bladder habits? Change in sexual function? for Change in menses?
- Knees: any popping, clicking, snapping? Knee ever locks? Swell? Give way?
Treatment previous
- Who did they see? When? What tests done?
- What diagnosis? What treatment? Did it help?
- Relevant injuries/x-rays
- When? What happened? Eventual outcome/residual certain activities? effects?
- Where x-rays taken? What were the results?
LORDFICARAH
Location : Where the pain and tenderness is
Onset: When the pain started
Referral Pattern: Does the pain refer – the behavior of the referral (e.g. numbness, tingling, shooting, burning etc…)
Duration: How long the pain lasts
Frequency: Is the pain constant or does it come and go?
Intensity: The severity of the pain the client is experiencing at the moment and at certain times of the day, moment of injury etc. The client may describe the pain as Mild, Moderate, Severe OR you may suggest using a pain scale. 1-10/10.
Character: Characteristic of the pain ( dull, shooting, achy, etc…)
Aggravating Factors: What makes the pain worse?
Relieving Factors: What makes the pain decrease or go away?
Alternative Healthcare: Other health care provider that the client has seen in relation to the complaint. ( MD, Chiro, Physio, Naturopath etc…)
Health History: This information will come from the Health History Form that the client fills out when they come in for the first time.
OLDERSAAB
Onset
Location
Description (what does it feel like)
Exacerbating factors
Radiation
Severity
Associated symptoms
Alleviating factors
Before (ever experience this before)
LOSTWAR
Location
Onset
Severity
Time
Worsening factors
Alleviating factors
Radiation
LMNOPQRSTTUVW
Location (where? point to it)
Modifying factors (what makes it better/worse)
Numbness, tingling or weakness
Onset of pain/illness (time, duration)
Palliative factors for pain
Quality of pain (throbbing, stabbing, dull, etc.)
Radiation (how does pain spread)
Severity of pain (usually scale of 1-10)
Timing of pain (after exercise, in evening, etc.)
Treatments tried
U: How does it affect ‘U‘ in your daily life? (ADL’s)
Deja Vu: Has this happened before?
Worry: What do you think or fear that it is?