Massage Therapy Palpation
Palpation is a fundamental technique used in massage therapy that involves using the hands to examine the body. It allows massage therapists to assess the condition of muscles, joints, and other tissues, helping them identify areas of tension, pain, and dysfunction. Effective palpation skills are crucial for delivering targeted and effective massage therapy treatments.
Clinical Application
Initial Assessment
Begin with light palpation to get an overall sense of the tissue condition, followed by deeper palpation to identify specific issues.
During Massage Treatment
Use palpation to monitor the effects of massage techniques and adjust pressure and methods as needed.
Post- Massage Treatment
Reassess the tissues to determine the effectiveness of the treatment and plan future sessions.
Points to Remember
- Maintain open communication with the patient to ensure comfort and receive feedback on tender areas.
- Use appropriate pressure and sensitivity to avoid causing pain or discomfort.
- Develop consistent palpation techniques to reliably assess and track changes in tissue condition.
- Continuously improve palpation skills through practice, study, and professional development.
Purpose of Palpation
- To assess tissue condition and to identify areas of muscle tension, spasm, or hypertonicity.
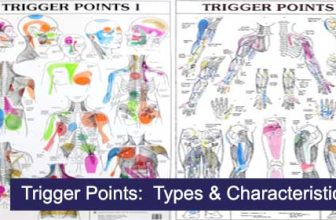
- To locate trigger points and to find and assess points of hypersensitivity that may cause referred pain.
- To precisely locate specific muscles that need to be targeted based on orthopedic assessment.
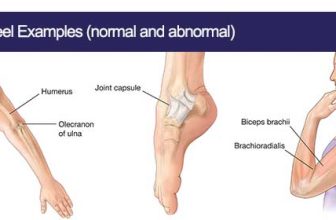
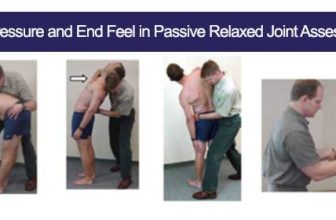
- To evaluate joint mobility and to determine the range of motion and any restrictions in the joints.
- To identify abnormalities such as lumps, swelling, or changes in tissue texture.
- To monitor treatment progress and track changes in tissue condition throughout and between treatments.
Palpation Techniques in Massage Therapy
Light Palpation:
The massage therapist uses the pads of their fingers to gently explore the surface of the skin and underlying tissues.
Purpose: To assess surface structures and detect superficial abnormalities.
Deep Palpation:
The massage therapist applies firmer pressure using the fingers or palms to reach deeper layers of tissue.
Purpose: To assess deeper structures such as muscles, tendons, and ligaments.
Static Palpation:
The massage therapist places their fingers or hands on a specific spot and holds the position to feel for changes in tissue texture or tension.
Purpose: To assess a specific area or structure without movement.
Dynamic Palpation:
The massage therapist moves their hands or fingers over the tissue, or asks the patient to move while palpating to feel for changes during movement.
Purpose: To assess the movement and function of tissues and joints.
Cross-Fiber Palpation:
The massage therapist moves their fingers perpendicular to the patient’s muscle fibers to feel for irregularities.
Purpose: To assess the condition of muscle fibers and detect adhesions or scar tissue.
Four T’s of Palpation
The Four T’s of Palpation is a concept used in massage therapy and other manual therapy disciplines to guide practitioners in assessing the characteristics of tissues during palpation. The Four T’s stand for Temperature, Texture, Tone, and Tenderness. Here’s a look at each of these components:
1. Temperature:
Assessment: Using the back of your hand or your fingertips, assess the temperature of the skin and underlying tissues.
Normal Finding:
- Consistent, warm temperature that is symmetrical across similar areas.
Abnormal Findings:
- Increased Temperature: Could indicate inflammation or infection.
- Decreased Temperature: Could suggest ischemia, poor circulation or vascular issues.
2. Texture:
Assessment: Evaluate the texture of the skin and underlying tissues by gently moving your fingers across the surface.
Normal Finding:
- Smooth and pliable skin with even texture.
Abnormal Findings:
- Rough or Dry Skin: May indicate dehydration or skin conditions.
- Thickened or Hard Areas: Could be scar tissue, fibrosis, or other abnormal tissue changes.
- Swelling: Edema is present. Edema may be hard during the acute stage, and boggy in the chronic stage.
- Adhesions: Adhesions feel as if the tissue is stuck together
- Crepitus: Crepitus is a palpable roughness in the joint or tendon that is noted with movement and sometimes accompanied by an audible “grating or crunching”
3. Tone:
Assessment: Assess the muscle tone by palpating the muscles both at rest and during slight contraction.
Normal Finding:
- Muscles should feel firm yet elastic and responsive.
Abnormal Findings:
- Increased Muscle Tone: May indicate spasm, hypertonicity, or guarding due to pain.
- Decreased Muscle Tone: Could suggest atrophy, weakness, or neurological impairment.
4. Tenderness:
Assessment: Check for areas of tenderness by applying gentle pressure and asking the patient to report any discomfort or pain.
Normal Finding:
Minimal or no tenderness in healthy tissues.
Abnormal Findings:
- Pain may be indicated if the patient winces or pulls away with tissue compression.
- Localized Tenderness: May indicate trigger points, inflammation, or injury.
- Diffuse Tenderness: Could be a sign of more widespread inflammation or systemic conditions.
Palpation Assessments and Findings
- Normal Tissue – Smooth, pliable, and consistent texture.
- Muscle Tension – Firmness, tightness, and possibly tender areas.
- Trigger Points – Small, hyperirritable spots that may refer pain when pressed.
- Swelling/Edema – Puffy, soft, and fluid-filled areas.
- Scar Tissue – Firm, irregular, and sometimes tender areas.
- Joint Restrictions – Limited movement, resistance, and possibly pain when moving the joint.
Common Pitfalls in Palpation for Tissue Assessment
- Lack of Concentration on What is Being Touched: Not fully focusing on the tactile sensations can lead to missing important details about the tissue condition.
- Too Much Movement of the Palpating Fingers: Excessive finger movement can interfere with accurately assessing the underlying structures and may result in an incomplete or inaccurate assessment.
- Using Excessive Pressure: Applying too much pressure can cause discomfort or pain to the patient and may obscure subtle differences in tissue texture and tone.
- Inconsistent Pressure: Varying the amount of pressure applied during palpation can lead to inconsistent findings and make it difficult to compare different areas accurately.
- Failure to Compare Bilaterally: Not comparing both sides of the body can result in missing asymmetries that could be significant for diagnosis and treatment.
- Ignoring Patient Feedback: Not listening to or considering the patient’s feedback regarding tenderness or pain can lead to overlooking critical information about the tissue condition.
- Palpating Too Quickly: Moving too quickly can prevent the therapist from thoroughly assessing the tissues and noticing subtle abnormalities.
- Insufficient Knowledge of Anatomy: A lack of detailed anatomical knowledge can hinder the therapist’s ability to accurately identify and interpret the structures being palpated.
- Palpating with Cold Hands: Cold hands can be uncomfortable for the patient and can also reduce the therapist’s sensitivity to the tissue’s characteristics.
- Lack of Systematic Approach: Not following a consistent, systematic method can result in missing important areas or inconsistencies in the assessment.
- Overlooking Subtle Changes: Failing to notice or dismissing small changes in tissue texture, tone, or temperature can lead to incomplete assessments.
- Inadequate Documentation: Not properly documenting findings can lead to difficulties in tracking progress and making informed treatment decisions.