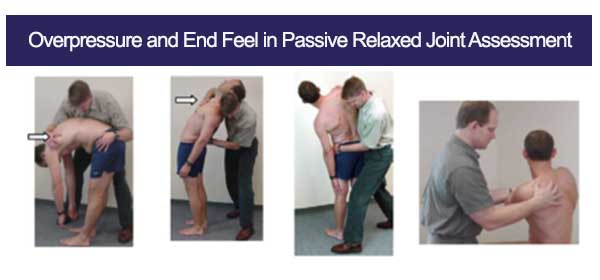
Overpressure Definition
Overpressure refers to the additional pressure applied by a clinician/ therapist at the end range of a passive movement to assess the integrity of the joint, the elasticity of the soft tissues, and to identify the end-feel.
Overpressure is the term used when the therapist gradually applies more pressure when the end of the available passive range of motion is reached. The sensation transmitted to the therapist’s hands by the tissue resistance at the end of the available range is the end feel of the joint.
The stretch on the soft tissues such as muscles, tendons, fascia and ligaments, as well as the arrangement of the joint surfaces, determine the range of motion of the joint, therefore, the joint’s normal end feel.
Overpressure Purpose
Overpressure is used for:
- Diagnostic Assessment
- To evaluate the end-feel of a joint after determining the passive ROM (range of motion) available in a joint.
- To assess joint and soft tissue integrity.
- To identify any restrictions or pain.
- To determine the quality and nature of the resistance at the end range of movement.
- To differentiate between different types of tissue restrictions (e.g., muscular, capsular).
- Treatment Planning
- Helps in determining the appropriate therapeutic interventions.
- Assists in identifying areas that need stretching, mobilization, or strengthening.
- Monitoring Progress
- To assess changes in range of motion and joint function over time.
- To evaluate the effectiveness of therapeutic interventions.
Points to Remember about Overpressure
- Ensure the patient is comfortable and in a relaxed position.
- Continuously seek patient feedback during the procedure to avoid causing pain.
- Record findings meticulously to track changes and inform treatment plans.
Overpressure Technique:
- Start with light pressure and gradually increase to assess resistance.
- Apply gentle but firm pressure at the end of passive movement to feel the resistance.
- Ensure the patient is relaxed to avoid muscle guarding which can affect the assessment.
Communication when performing Overpressure:
- Always explain the procedure to the patient before performing overpressure.
- Monitor patient’s facial expressions and verbal feedback during the procedure.
- Observe for signs of discomfort, pain, or apprehension.
- Feel for abnormal end-feels such as soft, firm, hard, empty, or springy block.
7 Contraindications to Overpressure
- Do not perform overpressure if the patient reports pain at the end range of motion. Pain during movement suggests inflammation, acute injury, or other pathology that could be exacerbated by overpressure.
- Avoid overpressure in joints that have recently undergone surgical procedures. Healing tissues are vulnerable and excessive force could disrupt the healing process.
- Do not apply overpressure if there is acute inflammation in the joint (e.g., due to rheumatoid arthritis or gout). Overpressure can worsen inflammation and cause more pain.
- Avoid overpressure on joints near a recent fracture or where a fracture is suspected. It can cause additional damage and pain.
- Do not apply overpressure to joints with known instability (e.g., due to ligament tears or severe laxity). It can increase the risk of further injury.
- Be cautious or avoid overpressure in patients with severe osteoporosis. Fragile bones can be easily damaged by excessive force.
- Use caution with patients having neurological conditions affecting muscle tone or control (e.g., spasticity). Abnormal muscle responses can be triggered by overpressure.
How to Perform Overpressure
- Position the Patient:
Ensure the patient is in a comfortable position where the joint being assessed can move freely. For example, if assessing shoulder flexion, the patient could be seated or standing. - Perform Passive Range of Motion (PROM):
Move the joint passively through its full range of motion without the patient actively engaging their muscles. This means the therapist moves the limb while the patient remains relaxed. - Apply Overpressure:
Once the joint reaches the end of its passive range of motion, apply a gentle but firm additional pressure.
This overpressure should be gradual and controlled to feel the resistance of the joint or tissues.
Maintain communication with the patient to monitor for any discomfort or pain.
End-Feel
End-feel is the quality of the resistance felt by the clinician at the end of a passive range of motion. It provides valuable information about the type of tissue limiting the motion and any potential abnormalities. End feel assesses the specific structure that is limiting movement or that is likely injured.
Normal end feel exists when the joint has full range of motion and the range is stopped by the anatomy of the joint.
Abnormal end feel exists when the range of the joint is less or greater than normal, is painful, or when a structure other than the normal anatomy of the joint stops the motion.
3 Types of Normal End Feel after Overpressure
-
- FIRM (Capsular Stretch/ Leathery End Feel): Characterized by a firm or springy sensation due to muscle, ligament, or capsular stretch.
- Feels like a a firm, springy sensation where the movement is stopped by muscle, ligament, or capsular stretch. It feels like stretching a thick rubber band.
- Example of Firm Normal End Feel: ankle dorsiflexion.
- HARD (Bony End Feel): When bone contacts bone, resulting in an abrupt stop to the movement.
- Feels like an abrupt, unyielding stop to movement due to bone contacting bone. It feels like tapping two solid surfaces together.
- Example of Hard Normal End Feel: elbow extension.
- SOFT: (Soft Tissue Approximation/ Muscular Stretch): Occurs when soft tissue approximation stops the movement, such as the contact between muscle and adipose tissue.
- Feels like a cushioned, soft sensation that stops the movement due to soft tissue contact. It feels like pressing a pillow against another pillow.
- Example of Soft Normal End Feel: elbow flexion.
- FIRM (Capsular Stretch/ Leathery End Feel): Characterized by a firm or springy sensation due to muscle, ligament, or capsular stretch.
5 Types of Abnormal End Feel after Overpressure
- EMPTY End Feel: No real end-feel because the patient stops the clinician due to pain, indicating inflammation, fracture, or psychogenic disorders.
- What it feels like: No actual end-feel because the patient stops the movement due to pain, before the clinician feels any resistance. It feels like a movement that is abruptly halted by the patient’s reaction.
- Example of abnormal empty end feel: Passive shoulder abduction where the patient experiences severe pain and stops the movement.
- SPRINGY BLOCK (Internal Derangement): A rebound effect indicating internal derangement like a meniscal tear in the knee.
- Feels like a rebound effect or a bouncy resistance occurring where it shouldn’t, indicating internal derangement. It feels like pressing down on a coiled spring that pushes back.
- Example of abnormal springy block end feel: Knee extension with a torn meniscus.
- FIRM (Capsular Stretch/ Leathery End Feel) : Occurs sooner or later in the ROM than usual, or in a joint that normally has a soft or hard end-feel. It can suggest increased muscle tone, capsular/muscular/ligamentous shortening.
- Feels like a firm, springy resistance occurring earlier or later than expected, or in a joint that normally does not have a firm end-feel. It feels like a shortened stretch or a prematurely taut rubber band.
- Example of abnormal firm end feel: Shoulder abduction with adhesive capsulitis (frozen shoulder).
- HARD (Bony End Feel): : Occurs sooner or later in the ROM than usual, or in a joint that normally has a soft or firm end-feel. It may indicate osteoarthritis, loose bodies in the joint, or a fracture.
- Feels like an abrupt, bony stop occurring earlier or later than expected, or in a joint that normally does not have a hard end-feel. It feels like hitting a hard surface sooner than anticipated.
- Example of abnormal hard end feel: Elbow extension with osteoarthritis.
- SOFT (Boggy): Occurs sooner or later in the ROM than usual, or in a joint that normally has a firm or hard end-feel. It can indicate edema or synovitis.
- Feels like a soft, boggy sensation occurring earlier or later than expected, or in a joint that normally does not have a soft end-feel. It feels like pressing into a water-filled balloon.
- Example of abnormal soft/boggy end feel: Knee flexion with significant swelling.