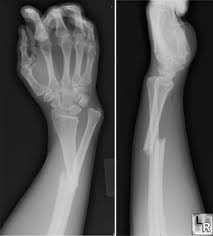
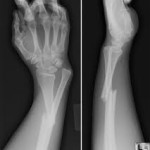
 A fracture is a break in the continuity of the bone. In fractures, there are associated soft tissue injuries to the Ligaments, muscles, tendons, fascia, nerves, blood vessels, skin. And cleint may have associated contusions, strains, sprains, dislocations at fracture site.
A fracture is a break in the continuity of the bone. In fractures, there are associated soft tissue injuries to the Ligaments, muscles, tendons, fascia, nerves, blood vessels, skin. And cleint may have associated contusions, strains, sprains, dislocations at fracture site.
Fracture Classification:
- Fractures are classified into several types depending on the type of break, location on the bone and angle of the broken ends
- If the skin is intact, it is termed CLOSED/ SIMPLE fracture
- If the ends of the bone have broken through the skin or into any of the body cavities, it is called an OPEN/ COMPOUND fracture.
- Fractures may be COMPLETE, where bone is broken into 2 or more pieces, or INCOMPLETE where bone is bent or cracked and periosteum remains intact
COMPLETE FRACTURES:
- Transverse Fracture — break in a straight line. They usually stay in place well after reduction ( put it back where it needs to be so its able to heal) , but they take longer to heal
- Oblique Fracture — break on an oblique ( diagonal ) angle. More difficult to keep in place even when splinted, but heals faster than transverse. ( more surface area).
- Spiral Fracture — fracture spirals up the long axis, wraps around the bone
- Comminuted Fracture — 2 or more bony fragments. Often unstable and the pieces make healing difficult.
- Avulsion Fracture — a ligament or tendon pulls away the portion of the bone it is attached to ( ex patellar tendon pulls away and takes tibial tuberosity with it)
- Osteochondral ( bone and cartilage) Fracture — fragments of articular cartilage are sheared from the joint surface.
INCOMPLETE FRACTURES:
- Compression Fracture — the bone is crushed. Happens in vertebral bodies
- Greenstick Fracture — bone is bent, partially broken. Happens in children younger than 10 years because bones are more pliable.
- Perforation Fracture — result of a missile wound such as a bullet
- Stress Fracture — cracks in the bone due to overuse and repetitive actions ( common in athletes)
Fracture Massage: CAUSES OF FRACTURES
- Trauma or force which creates more stress than bone can absorb
- Direct force — from object striking it, bone breaks on impact
- Indirect force — bone breaks at a distance from site of force. Torquing or twisting causes a spiral break.
- Overuse / repeated wear, causing cracks in bone
- Pathologies such as osteoporosis, tumours, local infections, bone cysts, anything causing bone weakness, brittleness.
Fracture Complications:
Early Fracture Complications:
- Compartment syndrome in leg/ forearm. Inflammation and hematoma increase pressure within fascial compartment
- Nerve compression — paresthesia beneath cast
- Vascular damage
- Bone / soft tissue infections
- DVT
- Pressure sore — from cast
Late Fracture Comlications:
- Delayed union — bone does not unite within expected time frame
- Non union — failure of bone to heal. May be due to large space between bone ends
- Malunion — unacceptable joining of bone ends, deformity occurs.
- Myositis ossificans — bone formation within a muscle following a hematoma
- Avascular bone necrosis — bone death due to poor vascularization
- Disuse osteoporosis — prolonged immobilization. Reversible once function returns
Fracture Massage: SIGNS & SYMPTOMS Of FRACTURE:
Immediately post-fracture, before reduction:
-  Unnatural mobility
-  Deformity
-  Shock
-  Bleeding
-  Inflammation, swelling, loss of function
-  Muscle splinting
-  Edema
-  Soft tissue damage — periosteum, ligaments, tendons, nerves, muscles fascia, skin
-  Stress fracture is painful upon compression
During Fracture Immobilization (when it is casted):
-  Possible incisions, pins, crutches, taping
-  Pain local and within a distance from site
-  Tissue repair at site, adhesions developing
-  Due to immobilization, decrease circulation, disuse atrophy, CT contracture in tissue under cast. Cartilage health decreased in joints below cast due to lack of successive action and circulation.
-  HT and TP in compensating structures
Fracture Immobilization Removed:
-  Fracture healing, remodeling
-  Decreased tissue health under cast. For the first few days after cast is removed, tissue is fragile and muscle tone lost
-  Adhesion matured around injury, connective tissue contractures. Pain stiffness in joints that were immobilized
-  Muscle weakness, disuse atrophy in muscles crossing site
-  Altered gait if in lower limb
-  Hypertonicity, trigger points in muscle crossing site
-  Pocket of chronic edema
-  Long term complications may occur now
Fracture Massage: OBSERVATIONS
During Fracture Immobilization:
-  Antalgic gait with lower limb fracture, antalgic posture
-  Affected limb casted
-  Crutches, cast, sling
-  Edema beneath cast at site, distal edema
-  Red, black, purple bruising beneath cast, distal
Fracture Immobilization Removed:
-  Habitual antalgic gait, posture
-  Chronic edema at site, distal
-  Skin beneath cast dry, scaly, flaky
-  Disuse atrophy
-  Bruising yellow, brown, green
Fracture Massage: PALPATION
During Fracture Immobilization:
-  Heat and edema below cast ( not palpable)
-  Pain local to fracture, nearby
-  Muscle spasm in muscle crossing site
-  Hypertonicity and Trigger Points in compensating muscles ( with upper limb, neck affected and unaffected shoulders ) ( with lower limb, pelvis, contralateral leg, shoulders due to crutch)
Fracture Immobilization Removed:
-  Tissue health assessed in the first few days — disuse atrophy, dry, flaky skin, parasthesia, lasting inflammation, edema, point tenderness around site
-  After one week, as tissue health returns, adhesions palpated around site
-  Hypertonicity and trigger points in muscles
Massage for Fractures: ORTHOPEDIC TESTING
 During Fracture Immobilization
- Testing of muscles directly involved in fractured is Contraindicated
- Active Free ROM of proximal and distal joints is assessed in pain-free ranges. Reduced ranges are likely
- Passive Relaxed ROM is performed with care. With upper limb fractures, cast is often removed after union but BEFORE consolidation. Therapist must not stress the repairing bone during testing
- Overpressure is Contraindicated until consolidation has occurred
- Active Resisted ROM may be performed gently. When cast is first removed, strength and tone are decreased.
Massage Therapy for Fractures: CONTRAINDICATIONS
 During Fracture Immobilization
- No traction before union has occurred
- No hot hydro distal or immediately proximal to cast — causes congestion under cast
- If fracture was a muscle attachment site, Active Free and Active Resisted Testing should only be performed with MD approval
- With open reduction ( surgical), on site work avoided until skin is healed
- With stress fracture, on-site work Cid while site is tender
 Fracture Immobilization Removed
- Overpressure contraindicated before consolidation
- No extreme temperature hydro on tissue under cast — perception of temperature may be altered
- No deep longitudinal technique on muscle until tissue health and muscle tone are regained. Passive stretch done carefully
- No hot hydro with pins or metal plates
 Generally, before 2 weeks, do not do too much, after two weeks the tissue health would get better
Fracture Massage Therapy Treatment: Procedure
 During Fracture Immobilization
- Cool hydrotherapy, applied distal to the cast
- Pumping to proximal lymph nodes, Manual Lymphatic Drainage proximal to the cast
- Limb proximal to cast treated with effleurage, petrissage, kneading to reduce pain, hypertonicity, as well as to increase drainage, venous return
- No traction before union occurs
- Mid-range pain-free Passive ROM to proximal and distal limbs
- Vibrations through cast can decrease SNS firing
- Work distal to cast restricted to light stroking, muscle squeezing, vibrations
- Treat secondary conditions ( strains, sprains)
 Fracture Immobilization Removed
Start the two-week count from when the cast was removed.
Not quite 2 weeks yet ( standard but not for everyone)
-  Mild contrast hydrotherapy ( to increase circulation) to tissue that was under cast
-  Proximal Manual lymphatic Drainage if edema still present
-  Proximal limb treatment to decrease Hypertonicity and Trigger Point
-  Stimulating, light techniques on muscle with atrophy. Gentle petrissage, muscle squeezing, shaking, point kneading, light tapotement
-  Pain free passive and active ROM — until tone has improved, do not put a stretch on muscles
-  Joint play on compensating joints
Around after 2 weeks ( standard but not for everyone)
-  As tissue health improves ( at least 2 weeks have passed since cast was removed) fewer modifications are needed. On site focus is on decreasing adhesion, scar tissue so ROM can increase
-  Chronic edema is reduced using fascial techniques followed by MLD
-  Once muscle tone has improved, therapist use effleurage, kneading, muscle stripping, cross fiber friction to adhesions around the site
-  Pain free passive stretch to muscles to re-align fibers
-  Trigger point treatments near the fracture site are treated
-  Once consolidation has occurred, joint play is indicated to joints beneath cast to restore ROM
-  Distal limb treatment with effleurage, petrissage to increase local venous return
Massage for Fractures: SELF CARE
 During Fracture Immobilization
- Limb elevated to reduce edema
- Seek a medical doctor’s attention for early complications such as increase in pain, heat, swelling
- Cool hydro to distal edema
- As soon as permitted by a medical doctor, strength and flexibility is maintained in compensating structures. Also, Active Free ROM of distal joints can begin with a medical doctor’s approval. May help to reduce atrophy
 Fracture Immobilization Removed:
- Limb is elevated to reduce remaining edema
- Mild contrast hydrotherapy on site
- Rem-ex continued for compensating structure
- Active Free ROM of joints beneath cast is perormed to onset of pain. If atrophy is minimal, client may begin Active Resisted exercises to regain muscle strength
- Self-stretches to regain ROM once consolidation has occurred
- Self massage to adhesion